BioLight Life Sciences Investments (OTCQX:BLGTY; TASE:BOLT) is now defining itself as an ophthalmology company after spending several years assembling a cluster of investments in the sector as well as in cancer diagnostics.
“We believe there is a huge value potential from the ophthalmic therapeutics and diagnostics we have gathered,” CEO, Suzana Nahum Zilberberg, says in an interview with BioTuesdays.com.
“These technologies target diseases with unmet medical needs that require innovation to treat large and growing patient populations, especially in the elderly,” she adds.
While BioLight intends to retain its controlling ownership position in its Micromedic cancer diagnostics portfolio, “on a daily basis, we are focusing on ophthalmology,” she contends.
BioLight’s game plan has the backing of a number of strategic investors, with a track record of biopharmaceutical success. They include Israel Makov, former president and CEO of Teva Pharmaceuticals; Dilip Shanghvi, founder and managing director of Sun Pharma, one of India’s largest pharma companies; Dan Oren, founder, president and CEO of Dexcel Pharma, a leading pharmaceutical manufacturer in Israel; and Rock One of Hong Kong.
BioLight’s current ophthalmic targets are glaucoma, dry eye syndrome (DES) and age-related macular degeneration (AMD).
Ms. Zilberberg explains that poor compliance and adherence with eye drops is a major clinical challenge in glaucoma treatment. Poor compliance occurs in an estimated 25% to 70% of patients, especially when drugs must be administered more than once daily.
BioLight’s solution is a long-term controlled release subconjunctival insert, called Eye-D, to reduce intraocular pressure. “This is a platform technology that can work with different active ingredients,” Ms. Zilberberg points out. The company’s first insert utilizes the market leading glaucoma generic drug, latanoprost.
The Eye-D insert is placed under the eyelid, just below the surface of the eye in a quick office procedure by an ophthalmologist and is invisible to the patient. The non-biodegradable insert can last for 12 months, after which it is removed and replaced with a new insert, she adds.
The company currently is conducting a first-in-humans study with up to 68 glaucoma patients at seven clinical sites in the U.S. to evaluate the safety and efficacy of three doses of a latanoprost insert over a duration of three months.
The Phase 1/2a study has three treatment arms and one control of arm, consisting of latanoprost eye drops. Results are expected in mid-2016. The FDA considers Eye-D to be a drug product and BioLight is pursuing a 505 (b) (2) regulatory approval pathway.
According to the American Glaucoma Society, there are about 10 million glaucoma patients in the U.S. Ms. Zilberberg figures the market potential of a latanoprost insert could reach billions of dollars in the U.S. alone. “Even a 5% market share translates into hundreds of millions of dollars in sales in the U.S.” she points out.
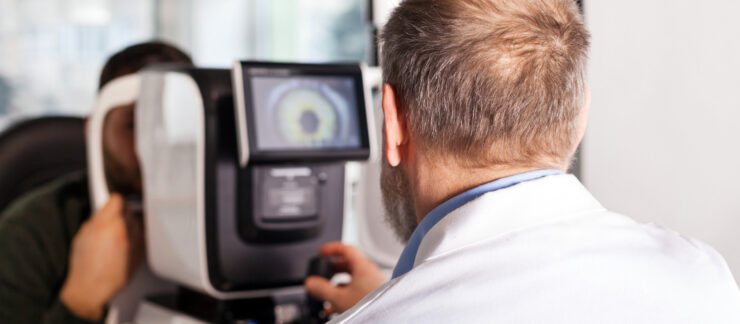
BioLight’s first commercial product is IOPtiMate, a CO2 laser technology that enables eye surgeons to reduce elevated intraocular pressure by thinning the white part of the eye, or sclera, without penetrating the eyeball.
IOPtiMate is a CO2 laser technology that enables eye surgeons to reduce elevated intraocular pressure by thinning the white part of the eye, or sclera, without penetrating the eyeball.
After existing glaucoma drugs are no longer effective, the current standard of care is laser trabeculoplasty or an invasive surgery called trabeculectomy. Both treatments are designed to relieve intraocular pressure, by punching holes in the eyeball, so that fluid can drain out of the front part of the eye.
“The IOPtiMate system transforms the current complex and highly risky glaucoma surgery into a safe and precise laser-assisted procedure,” Ms. Zilberberg contends. “The procedure provides high efficacy and allows for substantial reductions in post-operative complications and use of eye drops.”
Data from a multi-center clinical study performed on 111 patients, with a five-year follow up, demonstrated significant long-term reduction in intraocular pressure and stability over time, an extremely low post-operative complication rate and long-term reduction in medications.
IOPtiMate has been approved in Europe, China, Mexico, Peru and Israel, with Canadian approval expected in a few months. Recent marketing efforts have resulted in first sales in Hong Kong, Poland, Hungary, Romania and Peru. She says distribution agreements are being negotiated in additional countries.
Last month, BioLight arranged a joint financing agreement with two Asia-based venture capital firms to continue the global commercialization of IOPtiMate and initiate a U.S. regulatory approval pathway process for the device in early 2016.
“Interest in IOPtiMate and its clinical benefits continues to spread among clinicians, patients and payers around the world, and this investment will allow us to continue to drive global awareness and commercialization of this innovative surgical system,” Ms. Zilberberg suggests.
Some 20 IOPtiMate systems have been installed worldwide, with more than 1,500 procedures performed to date.
Since many glaucoma patients tend to DES, BioLight also is developing a multi-parameter diagnostic test for the analysis of tear film.
Dry eye is a multifactorial disease of tear film and the ocular surface that results in symptoms of discomfort, visual disturbance, and tear film instability with potential damage to the ocular surface.
More than 100 million people suffer from moderate-to-severe DES worldwide, of which 20 million to 40 million are in the U.S., with different levels of severity. DES is the largest single reason for visits to eye doctors in the U.S.
Ms. Zilberberg explains that BioLight’s TeaRx device is a multi-parameter, cost effective solution to DES. “It is a rapid and easy to use diagnostic test that will be able to identify the origin of the condition for targeted therapy and can be used by any health care professional. TeaRx could be a combined solution of a diagnostic test with a specified therapy or be used as a standalone kit.”
There is currently one FDA-approved drug for DES, Restatis, which targets only a subgroup of patients.
“This is a very heterogeneous population, so there is strong demand for personalized treatment and companion diagnostics solutions,” she adds. “We hope to use our diagnostic to collaborate with drug development companies to help expand the number of treatment options.”
In an earlier U.S. clinical trial, BioLight’s development partner, Ora Inc., demonstrated a significant correlation of DES benchmark tests to TeaRx’s parameters. A second clinical trial is assessing the sensitivity and specificity of TeaRx’s ability to diagnose dry eye patients.
“We hope to be in the market with this product in 2017,” Ms. Zilberberg suggests.
BioLight’s newest technology is the OphRx drug-delivery platform that is based on lyotropic liquid crystals and is designed to improve the transport of therapeutic molecules across ocular membranes.
OphRx is currently in preclinical development and the company hopes to release data in the first half of 2016.
BioLight is following two pathways with OphRx. One is to determine if the platform can transport topically-administered medications to replace back-of-the-eye injections for the treatment of AMD. The other is determine if the platform can improve safety and efficacy of front-of-the-eye medications for the treatment of DES and glaucoma.
“The molecular structure of the liquid crystals is very flexible,” Ms. Zilberberg says. “We believe we can control the penetration of molecules across ocular membranes and provide controlled-release medications.”