For the first time in a century, administration of epidural needles is being transformed with a smart device developed by closely-held Omeq Medical, which has completed a proof of concept (POC) preclinical study, is currently preparing for FDA submission, and expects to initiate first-in-human trials later this year.
“Our device integrates with standard syringe and needle kits to turn them into smart needles that alert physicians with visual indications once the needle penetrates into the right spot, and prevents overshooting into the spine,” Lior Margalit, co-founder and CEO, says in an interview with BioTuesdays.
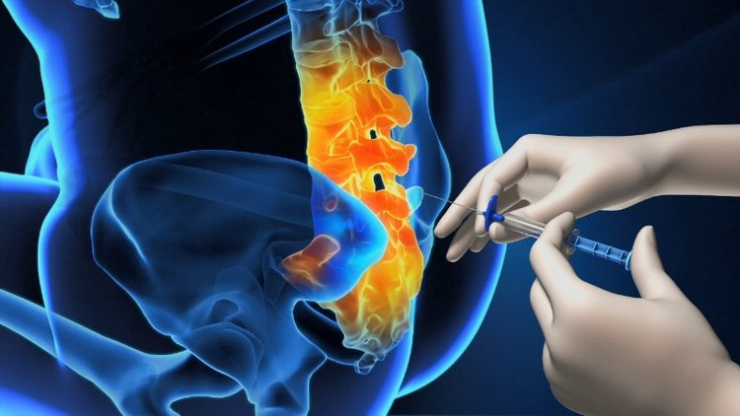
A traditional epidural injection procedure involves the delivery of drugs such as anesthetics and steroids, into the four-millimeter space that contains fat cells and small blood vessels around the spinal cord, called the epidural space.
The procedure requires extensive physician training and relies heavily on tactile feedback, and the loss of resistance (LOR) technique, in that once the needle passes through the ligaments of the spine and enters the epidural space, the physician feels a change in pressure that indicates the epidural space has been reached.
“When people think of epidurals, labor pain in pregnant women is what usually comes to mind,” Mr. Margalit points out. “In fact, globally each year most epidurals are used in surgical procedures by anesthesiologists, and in acute and chronic pain management.”
It is estimated that over 40 million epidural injections are administered annually throughout the world with inaccurate initial needle placement occurring in up to 30% of those cases, resulting in ineffective drug delivery, multiple insertions, and post-complications such as severe headaches, nerve damage and paralysis, he contends.
“Several years ago, when my father was undergoing orthopedic surgery the physician made three attempts at inserting the epidural needle,” Mr. Margalit recalls. “During one of those attempts, the physician punctured my father’s spine and, as a result, he suffered severe post-complications of headache, pain and nerve damage resulting in a lengthy hospital stay.”
As a biomedical engineer, this personal experience prompted Mr. Margalit to find a better way of administering epidural injections. “Clearly, there is a need for safer and more accurate epidural injections as the epidural space is narrow and hard to find leaving room for error, especially for younger physicians with less experience.”
The Omeq Medical smart device for epidural injections is a sensor-based, single-use epidural placement system for safe, accurate epidural injections, Mr. Margalit explains. “Our simple, easy-to-use device fits between a standard needle and syringe, and is compatible with most commonly used models on the market.”
The device gives automatic visual signals with LED lights that indicate correct needle placement, and continuously monitors tissue resistance at the needle tip, he says.
“In conjunction with LOR technique, a special blunted probe repeatedly protrudes from within the needle tip and monitors the resistance of the surrounding tissues to accurately detect, needle penetration into the epidural space,” Mr. Margalit describes.
Israel-based Omeq Medical has successfully completed a POC preclinical study at Assaf Harofe Hospital in Israel and is now moving toward clinical trials explains Mr. Margalit. “We are very encouraged by our POC results and are planning first-in-human clinical trials in Israel to commence by the end of 2018.”
With regard to FDA approval, Mr. Margalit says Omeq Medical is in the process of finalizing the file and plans to submit in a few weeks from now. “We anticipate FDA clearance in 2019.”
Results from the preclinical study will be part of the company’s FDA submission, he adds.
In addition to the potential for poor patient outcomes, multiple epidural insertions increase OR time and therefore, increase hospital costs because up to 30 minutes is generally required per epidural injection procedure.
Mr. Margalit points out that in the area of pain management, the current standard practise is to use image-guided, or x-ray machines, to accurately place epidural needles in order to administer a corticosteroid injection. “A physician may complete between 10-to-15 image guided procedures in a day, so exposure to radiation is a real issue,” he says.
Omeq Medical hopes to reduce the need for image-guided epidurals and in the future, plans to provide more clinical data in support of their device as a viable, safe alternative to image-guided epidurals, Mr. Margalit suggests.
“Our smart technology, assists physicians in giving safe and accurate epidural injections that result in improved time and cost efficiencies for hospitals, and most importantly, better patient outcomes,” he adds.
• • • • •
To connect with Omeq, or any of the other companies featured on BioTuesdays, send us an email at [email protected].